Tissue engineered hearts and lungs may be still at the laboratory stage, but replacement vaginas made from the patient’s own cells have been around for a while. A paper in the Lancet confirms they continue to work years after surgery.
The four patients in the study had Mayer-Rokitansky-Kuster-Hauser (MRKH) syndrome, which affects women who are genetically and hormonally normal but have an absent or greatly shortened vagina. MRKH may also produce a missing or defective cervix and uterus. Sex is usually painful for women with the condition and more than half a million are affected worldwide.
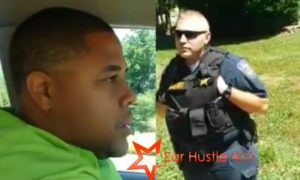
While we are some way from being able to enable women most with MRKH to conceive, the Wake Forest School of Medicine created sheets from biodegradable scaffolds and epithelial and muscle cells of four girls aged 13-18 with MRKH. These were then “hand-sewn into a vagina-like shape” in the authors’ words and implanted. Each vagina was shaped by the Federico Gomez Children’s Hospital, Mexico, to best match the body of the woman it was for.
Follow-ups over the next 6-8 years using physical examination, tissue biopsies and MRIs indicated that blood vessels had connected to the implant and within months new cells formed spontaneously while the scaffold was slowly absorbed. A tri-layered structure remained in place after the scaffolding was gone and no abnormalities were observed. The women responded to a questionnaire with responses in the normal range in regard to arousal, lubrication, orgasm and painless intercourse. Most significantly, the patients reported high satisfaction with the replacement vaginas.
Other existing treatments for MRKH are much more traumatic and have a high rate of failure and complication. Team leader Anthony Atala has used a similar technique to build replacement bladders for nine children in need, and has implanted urethras in boys, although there is yet to be the long-term confirmation of success in that case.
This pilot study is the first to demonstrate that vaginal organs can be constructed in the lab and used successfully in humans,” Atala said. “This may represent a new option for patients who require vaginal reconstructive surgeries. In addition, this study is one more example of how regenerative medicine strategies can be applied to a variety of tissues and organs.”
“I truly feel fortunate, because I’ll have a normal life,” a patient who wished to remain anonymous said in a video provided by the Federico Gomez Hospital . “It’s important to let other girls that have the same problem know that it does not end knowing that you have the disease, because there is a treatment.” Besides MRKH the process could be suitable for women whose vaginas have been damaged in trauma or by cancer. The announcement has generated excitement in the trans community.
Source: iflscience.com
[AdSense-A]








































































































































































































































![[Video] Chicago Police Officers Caught On Video Telling Two Black Men "We Kill Mother F**kers"](https://earhustle411.com/wp-content/uploads/2018/07/evil-cop-3-300x180.jpg)
![[Video] Chicago Police Officers Caught On Video Telling Two Black Men "We Kill Mother F**kers"](https://earhustle411.com/wp-content/uploads/2018/07/evil-cop-3-80x80.jpg)












![[Video] White Woman Calls The Cops On Black Real Estate Investor, Cops Threaten To Arrest Her For Harassing Him](https://earhustle411.com/wp-content/uploads/2018/05/nosy-neighbor-300x180.png)
![[Video] White Woman Calls The Cops On Black Real Estate Investor, Cops Threaten To Arrest Her For Harassing Him](https://earhustle411.com/wp-content/uploads/2018/05/nosy-neighbor-80x80.png)


![White Scientist Says The Black Community Is Being Targeted By The Medical System, They Are Deliberatly Being Poisoned [Video]](https://earhustle411.com/wp-content/uploads/2016/05/mike-adams-300x180.jpg)
![White Scientist Says The Black Community Is Being Targeted By The Medical System, They Are Deliberatly Being Poisoned [Video]](https://earhustle411.com/wp-content/uploads/2016/05/mike-adams-80x80.jpg)







![Teenage Girl Shot In Her Stomach Three Times But Took Time To Post To Facebook [ Video]](https://earhustle411.com/wp-content/uploads/2016/02/Gangster-chick-300x180.jpg)
![Teenage Girl Shot In Her Stomach Three Times But Took Time To Post To Facebook [ Video]](https://earhustle411.com/wp-content/uploads/2016/02/Gangster-chick-80x80.jpg)